Argininosuccinic aciduria (AA) and Citrullinemia
Clinical information
Argininosuccinic aciduria and citrullinemia are urea cycle disorders (UCDs). There are several of these disorders, and they all involve the same problem: inability or reduced ability to remove ammonia from the blood. Too much blood ammonia causes a variety of serious medical problems that may begin with irritability and refusal to eat/feed. Vomiting and increasing lethargy often follow, and infants may not be able to control body temperature (in particular, temperature may drop). The next problems to occur are often seizures, hypotonia (floppiness), breathing difficulties, neurologic posturing, and coma. These problems happen because the nervous system is very sensitive to excess ammonia. In patients with severe cases, the manifestations of disease begin in the first two days of life, with a normal appearnace at birth. Clinicians and others may also wish to read reference 1, which has a detailed description of the UCDs (1).
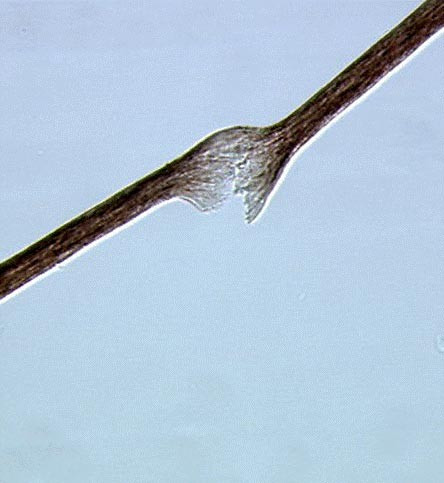
In technical terms, hyperammonemia causes cerebral edema, which compromises neurologic function. The immaturity of the neontal liver exacerbates the problem and the disease has a rapid clinical course. Quick disagnosis and treatment are the most effective ways to improve patient outcomes. We have not found any information suggesting that people with UCDs have special facial characteristics, apart from the fact that many have hair abnormalities (see photo below). Otherwise, the following problems may occur in AA and citrullinemia:
- Feeding difficulties
- Lethargy or drowsiness
- Vomiting
- Hypotonia (floppiness)
- Seizures
- Coma
- Hepatomegaly (enlarged liver)
- Liver disease/damage
- Brain atrophy
- Delays of motor development
- Intellectual disability
- Hair abnormalities (sparse or brittle hair, hair shaft abnormalities)
There are a variety of strategies for managing UCDs. Maximizing calorie intake appears to be an important factor in stabilizing patients, and enteral feeding of low-protein foods/foods with low amino acid content has been recommended (2). The advice of a nutritionist is important in this regard. In the case of AA and citrullinemia, additional approaches include arginine supplements and pharmaceutical agents that treat hyperammonemia. Clinicians and others are advised to consult the management guidelines for UCDs before making decisions about treatment options, as the information on this page is not exhaustive (2). The National Urea Cycle Disorders Foundation has also created also an information page on managing UCDs.
Argininosuccinic aciduria usually manifests in the first few days after birth, with signs and symptoms like those described above (irritability, lethargy/lack of energy, feeding problems, breathing problems, and body temperature problems. Seizures, neurologic posturing (unusual body movements or positions), and coma may follow. Some people with AA have a mild form of the disorder. In these people, ammonia only builds up in the blood during times of illness or other stresses. In some cases, blood ammonia may rise after eating. (3) In late-onset cases, delayed speech acquisition is an common problem (4).
Hair abnormalities in AA vary with the severity of the disease and a patient's nutritional status. There is evidence showing that dietary management, including arginine supplements and a low protein diet, can help hair become normal (5). Hair problems may also diminish as patients age.
There are two forms of citrullinemia (type 1 and type 2). Their clinical appearances are are different, and they are caused by mutations in different genes. Our software currently has data for citrullinemia type 1, which is also called classic citrullinemia. Patients with citrullinemia type 1 lack an enzyme called argininosuccinate synthetase (ASS). This enzyme helps remove nitrogen from the body, and too little of it allows ammonia to build up in body fluids, including blood. Medical problems resulting from ammonia buildup usually appear soon after birth (usually within days, although milder forms may not be evident until childhood or the teenage years). These problems are similar to those in the list for AA (feeding problems, lack of energy, etc.). Like AA, citrullinemia can be life-threatening. Type 1 citrullinemia is the most common form of this disease.
Type 2 citrullinemia can occur in infants, children, or adults. It can be triggered by It causes confusion, restlessness, memory loss, and behavior abnormalities that include agressiveness and hyperactivity. Like AA and type 1 citrullinemia, it can also cause seizures and coma, and can be life-threatening.
Diagnosis and Testing
AA and citrullinemia are inherited as autosomal recessive disorders (meaning, they result from gene mutations, and both parents contribute a mutated gene). As noted above, there do not appear to be special facial characteristics associated with either of these conditions, and laboratory values are helpful for diagnosing these disorders. According to accepted guidelines for managing UCDs (5), the following results are strong indicators of a UCD:
- Plasma ammonia is 150 micromoles per liter or higher
- There is a normal anion gap
- Blood glucose is normal
Gene sequencing is available to confirm a diagnosis of AA or citrullinemia. For a list of labs that do this type of testing, see the links at the right on this page.
References
- 1. Summar M (2001). Proceedings of a consensus conference for the management of patients with urea cycle disorders. J Pediatr 138(1 Suppl):S6-10. Abstract on PubMed Full text from rare Disease Network.
- 2. Summar M (2001). Current strategies for the management of neonatal urea cycle disorders. J Pediatr 138(1 Suppl):S30-39. Abstract on PubMed Full text from rare Disease Network.
- 3. Lagas P et al. (1991) Late onset argininosuccinic aciduria in a paranoid retardate. Biol Psych 30(12):1229-1232. Abstract on PubMed.
- 4. Billmeier GJ Jr et al. (1974) Argininosuccinic aciduria: investigation of an affected family. J Pediatr 84(1):85-89. Abstract on PubMed.
- 5. Kvedar JC et al. (1991) Dietary management reverses grooving and abnormal polarization of hair shafts in argininosuccinase deficiency. Am J Med Genet. 40(2):211-213. Abstract on PubMed.