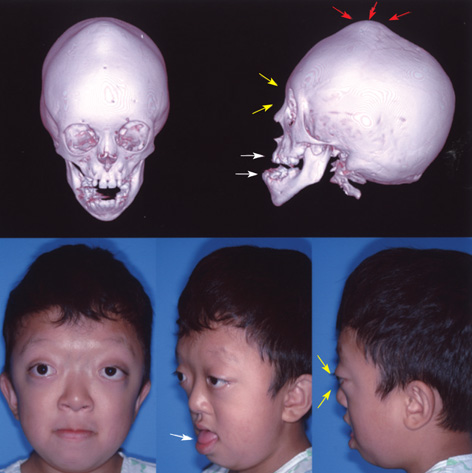
Pfeiffer syndrome
Pfeiffer syndrome is member of a group of disorders involving craniosynostosis. This term means that at least one of a person's skull bones fuses prematurely. The problem is often noted at birth, but it may be picked up on an ultrasound or it may not become evident until well after birth. Premature fusion of skull bones restricts skull growth, causing it to expand unevenly to accomodate brain growth.
When only one brain suture is closed prematurely, a person is said to have isolated craniosynostosis. This condition is relatively common, occuring in roughly 3-5 per 10,000 births or even more frequently (1, 2). Severity varies widely, with some cases being severe and others being barely noticeable. The causes for isolated craniosynostosis are not fully understood, but hereditary/genetic components are involved (1, 3). Possible risk factors for craniosynostosis include, but are not limited to, the mother's age and race more common among older women and whites); 4), male sex (4), and heavy maternal smoking, especially after the first trimester (5).
In addition to isolated craniosynostosis, there are also a number of craniosynostosis syndromes. As the name implies, the syndromic forms of craniosynostosis involve problems in a variety of body systems. The hands and/or feet are often affected, a fact that implies that skull and hand/foot development share some type of common mechanism. Apert syndrome is a member of a group named FGFR-related craniosynostosis syndromes. All members of this group are caused by mutations in the genes FGFR1, FGFR2, or FGFR3. In addition to Apert syndrome, the group includes Apert syndrome, Crouzon syndrome, Crouzon syndrome with acanthosis nigricans, Muenke syndrome, Jackson-Weiss syndrome, Beare-Stevenson syndrome, and FGFR2-related isolated coronal synostosis. Generally speaking, skull abnormalities in these syndromes are observed in the newborn period or before, although some cases may not be noted until later infancy or afterward. In addition to having abnormally shaped skulls, people with these syndromes tend to have wideset eyes that protrude outward (proptosis), an underdeveloped midface (hypoplasia; best seen in profile; see photos on this page), a small nose that may be beaked, and a highly arched palate or a cleft palate (see photos on this page). Intellectual disability is common, but does not always occur.
Clinical information
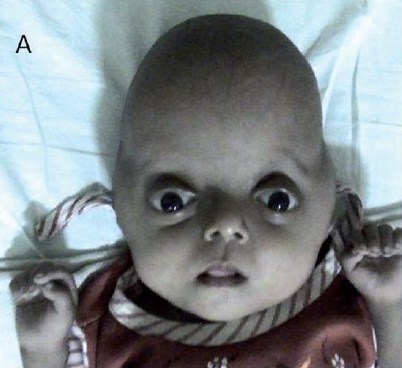
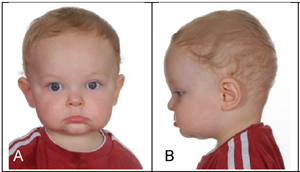
PS ranges in severity from mild to severe. The young girl in the photo at the right is likely severely affected, while the male infant at the bottom of this page was mildly affected.
The following are signs and symptoms of Pfeiffer syndrome. Because PS overlaps with other craniosynostosis syndromes, laboratory testing may be required to make a definitive diagnosis.
- Craniosynostosis (premature fusion of the skull bones, accompanied by unusual skull shape
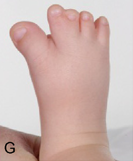
- Big toe or thumb points away from other digits (see photos below)
- Syndactyly (fusion of fingers or toes; see photo below)
- Large thumb or end of thumb is wide and/or squared
- Airway obstruction and/or respiratory difficulties
- Hydrocephalus (fluid buildup in the brain)
- Highly arched palate (see photos below)
- Delayed development of motor skills
- Intellectual disability
- Large big toe
- Hearing loss
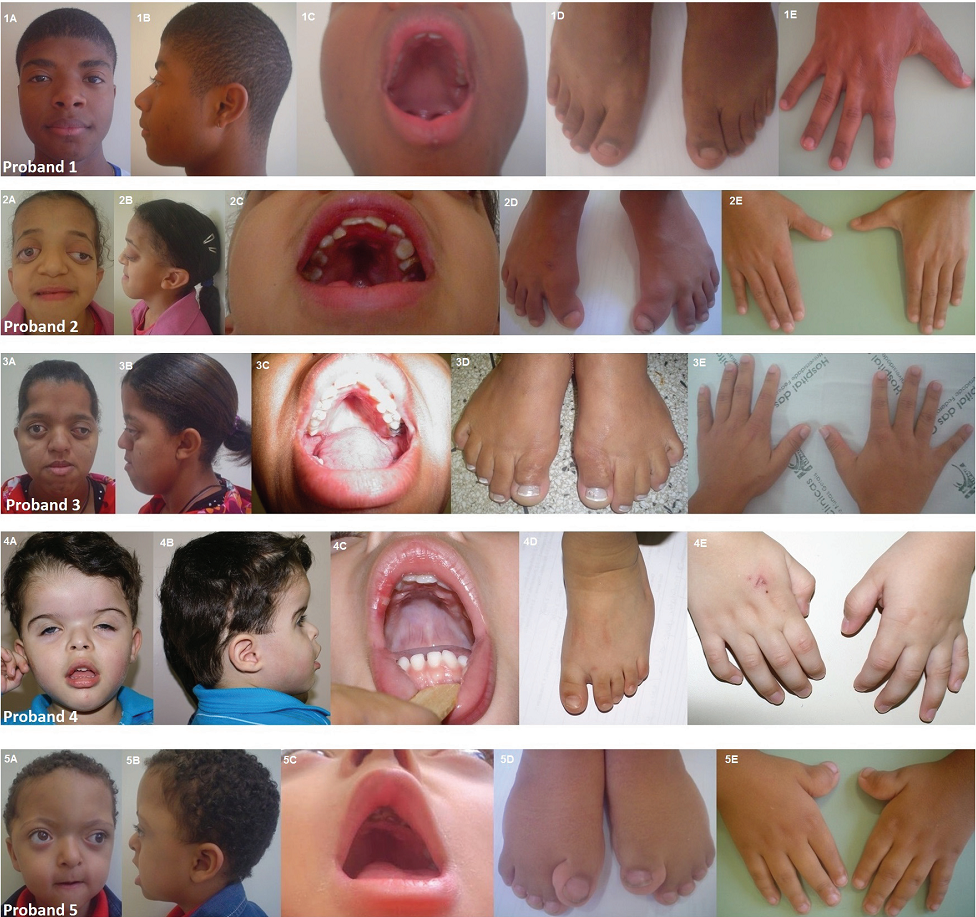
Common clinical features of Pfeiffer syndrome
In addition, PS and craniosynostosis patients often share a similar facial appearance. In addition to skull deformities, they may have the following facial features:
- Midface hypoplasia (the area between the eyes and the jaw is underdeveloped)
- Hypertelorism/wide-set eyes
- Proptosis/protruding eyes
- Nasal abnormalities
- Facial assymetry
- Large forehead
- Low-set ears
Facial features in Pfeiffer syndrome
Exophthalmos can be severe and may impair vision.
PS is an autosomal dominant disorder. This term means that it can be passed from one affected parent to a child. Given the severity of some forms of the condition, this mode of transmission generally occurs in type 1 patients. In patients without a family history of PS, the mutation arises spontaneously. Craniosynostosis syndromes are caused by mutations in the genes FGFR1, FGFR2, and FGFR3. The Gene Review article (see link at right) notes that all cases of types 2 and 3 are caused by mutations in FGFR2, while 95% of type 1 cases result from mutations in this gene. The remaining cases are caused by mutations in FGFR1. FGFR3 has not been associated with Pfeiffer syndromem Mutations in this gene cause Crouzon syndrom without acanthosis nigricans and Muenke syndrome. All other craniosynostosis syndromes are caused by mutations in FGFR2. The link at the right provides information about labs that test for mutations in these genes.
Pfeiffer syndrome has traditionally been classified into three groups (types 1, 2, and 3). Types 2 and 3 are the most serious forms of the syndrome. Type 1 PS is often called classic PS. The manifestations tend to be mild, and neurological and intellectual development are normal. These skulls of type 1 patients tend to be short from front to back and long from bottom to top. Patients with type 2 PS have cloverleaf skull abnormalities and developmental delays and neurological problems. The course of type 3 PS is similar to that of type 2, but it does not involve cloverleaf abnormalities. Readers may wish to read a review on Pfeiffer syndrome (1).
A recent publication proposed a new functional classification scheme for PS (2). Rather than using anatomical differences as the basis for grouping patients, the new scheme uses the terms mild, moderate, and severe. Patients are scored based on the presence or absence of different problems. Higher scores translate to more severe forms of disease:
Problem |
Score | ||
Respiratory |
Respiratory crisis or
|
3 |
|
Obstructive sleep apnea; no crisis |
2 |
||
Ocular |
Globe herniation |
3 |
|
Corneal exposure |
2 |
||
Amblyopia/strabismus |
1 |
||
Otologic |
Hearing impairment |
1 |
|
Neurologic |
Elevated intracranial pressure/
|
3 |
|
Chiari/syrinx/seizures/hydrocephalus/
|
2 |
||
Motor/speech delay |
1 |
Patients scoring 0-2 are classfied as mild. Scores of 3-5 are moderate, and patients with scores of 6-10 are considered to be severely affected.
The differential diagnosis for PS includes certain other craniosynostosis syndromes (most notably Apert syndrome and Crouzon syndrome). The Gene Review on the craniosynostosis syndromes (see link at right) has a list of other conditions that are part of the differential diagnosis for this group as a whole. They include a number of conditions.
References
- 1. Vogels A & Fryns JP (2006) Pfeiffer syndrome. Orphanet J Rare Dis 1:19. doi: 10.1186/1750-1172-1-19. Full text on PubMed.
- 2. Greig AV et al. (2013) Pfeiffer Syndrome: Analysis of a Clinical Series and Development of a Classification System. J Craniofac Surg 24(1):204-215. Abstract on PubMed.
- 3. Júnior HM (2015) Pfeiffer syndrome: Clinical and genetic findings in five Brazilian families. Med Oral Patol Oral Cir Bucal 20(1):e52-58. Full text on PubMed.
- 4. Chung J et al. (2008) Monoblock Craniofacial Internal Distraction in a Child with Pfeiffer Syndrome: A Case Report. J Kor Med Sci 23(2):342-346. Full text on PubMed.
- 5. Jay S et al. (2013) The fibroblast growth factor receptor 2 p.Ala172Phe mutation in Pfeiffer syndrome--history repeating itself. Am J Med Genet A 161A(5):1158-1163. Full text on PubMed.
- 6. Singh RK et al. (2010) Common primary fibroblastic growth factor receptor-related craniosynostosis syndromes: A pictorial review. J Pediatr Neurosci 5(1):72-75. Full text on PubMed.